HEADACHES
 By: Dr. Rachel Jakubowski
By: Dr. Rachel JakubowskiPhysical Therapist
SPECTRUM, Inc
Headaches are the most prevalent pain disorder, affecting 66% of the global population.
The International Headache Society describes several different categories of headache:
- Tension-type
- Cervicogenic
- Migraine and cluster
- Secondary headaches from an underlying condition (fever, infectious disease, sinus disorder, tumors)
- Cranial neuralgias, facial pain, and other headaches
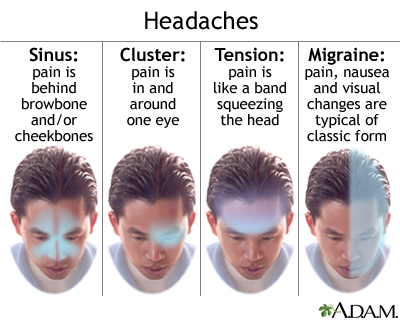
Tension-type headaches are the most common types of headaches in adults with research suggesting anywhere from 30 to 80% of adults in the US experiencing this type of headache. They are caused by stress, poor posture, fatigue, neck or jaw pain, dysfunctional breathing patterns, etc. The individual with tension-type headaches typically feels an ache or band-like pressure around the head, such as at the temples, above the eyes, or the back of the head and neck. These headaches can last for 30 minutes to several days and typically occur on both sides of the head (can occur unilaterally however).
Your neck muscles attach into the cervical spine or somewhere along your skull. In a way the muscles are tugging on your skull and creating so much “tension” that you end up developing a headache. And depending on which neck muscles get tight, you will get the feeling of pressure along the base of your skull, your forehead, or above your eyes.
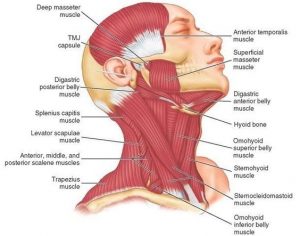 Common Muscles that can tighten and produce headache symptoms include:
Common Muscles that can tighten and produce headache symptoms include:
- Upper Trapezius
- Sternocleidomastoid
- Levator Scapulae
- Sub occipitals
- Scalenes
- Upper Trapezius
Over-counter medications such as Tylenol, Advil, Motrin, and Aleve can be used as needed but consult your doctor first and only when necessary. Only take the smallest dose needed to relieve your pain because sometimes overusing pain medications can cause rebound headaches.
Cervicogenic headaches differ from tension type headaches because they arise primarily from musculoskeletal dysfunction in the upper three cervical spine segments (zygoapophyseal/facet joints). Nerves that originate from your cervical spine supply motor and sensory information to skin and muscles at your head and neck. Pain receptors that lie along the same path can sometimes get stimulated and cause pain signals to be sent, which can then mimic headaches or neck pain.
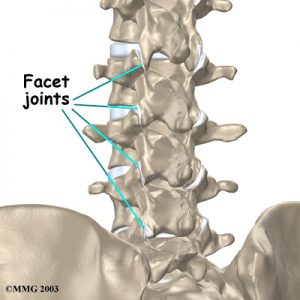 Identifiers of Cervicogenic pain:
Identifiers of Cervicogenic pain:
- Headache mainly felt on one side of the head (can at times occur on both sides of the head)
- Restricted neck range of motion
- Provocation of usual head pain by neck movement or sustained awkward neck positions
- Provocation of usual head pain with pressure applied over the upper cervical spine or base of the skull
- Vague same sided neck, shoulder or arm pain
Research has shown that neck exercises, specifically low-intensity endurance training, and spinal mobilizations were effective in the short-term and long-term for prognosis of Cervicogenic headaches.
The key is to remember that not all headaches are the same; you can get a headache from factors such as dehydration or sleep deprivation. The good news is that not all headache types require dependency on medications and most of the time if you figure out the cause and type of the headache you reduce your symptoms. Sometimes an injection of local anesthesia into the spine may be required but not in all cases. Physical therapists are are great resource to address tension type and cervicogenic headaches. Otherwise, consult with a neurologist or primary care physician to determine the underlying root of your headache.
Below are recommended exercises to reduce tension-type and cervicogenic headaches. You will need to stick to this program for at least 6 weeks, perform 1-2x/day.
Neck Stretches
- Upper Trapezius Stretch
- Levator Scapulae Stretch
- Scalene Stretch or SCM stretch
Neck Strengthening
- Chin Tuck
Shoulder Girdle Strengthening
- Prone T
- Prone Y
References:
American Migraine Foundation. Accessed 6/24/16
https://americanmigrainefoundation.org/living-with-migraines/types-of-headachemigraine/tension-type-headache/
Cervicogenic Headaches: An Evidence-Leg Approach to Clinical Management. Accessed 7/1/16
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3201065/
Cleveland Clinic. Tension Headaches. Accessed 7/5/16.
Clinical Evaluation of Cervicogenic Headache: A Clinical Perspective. Accessed 7/1/16.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2565113/?tool=pubmed.
National Headache Foundation. Tension-Type Headache. Accessed 7/5/2016.
You are… The bomb.com!!